-
 Pangea
Pangea
-
 Gustatory
Gustatory
-
 Telepoint base station
Telepoint base station
-
 Freshwater
Freshwater
-
 Blog
Blog
-
 Maintenance
Maintenance
-
 RIR
RIR
-
 Ununoctium
Ununoctium
-
 Block cipher
Block cipher
-
 Ailanthus
Ailanthus
-
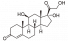 Corticosteroid
Corticosteroid
-
 Axial
Axial
-
 Hercules globular cluster
Hercules globular cluster
-
 Lagrangian point
Lagrangian point
-
 Heat stability
Heat stability
-
 Spreadsheet
Spreadsheet
-
 Falconiformes
Falconiformes
-
 Drag force
Drag force
-
 Alkalosis
Alkalosis
-
 Sierra
Sierra
-
 M 37
M 37
-
 Mammography
Mammography
-
 Internet
Internet
-
 Hemiptera
Hemiptera
-
 Genetic Engineering
Genetic Engineering
-
 Microfluidics
Microfluidics
-
 Iron bloom
Iron bloom
-
 Eris
Eris
-
 Pelvis
Pelvis
-
 Full Duplex
Full Duplex
Avian influenza
Avian influenza caused by the influenza virus strain A is an infectious disease affecting birds. It was identified for the first time in Italy more than 100 years ago and occurs throughout the whole world.
The disease in birds: impact and ways to combat it
All birds are believed to be sensitive to the infection although some species are more resistant that others. It can have a very wide range of symptoms from a benign form to a very contagious, rapidly fatal disease that causes serious epidemics. In this case we refer to highly pathogenic avian influenza which is of a sudden onset with serious symptoms and rapidly progresses to death with a death rate approaching 100%.
Fifteen sub-types of the influenza virus are known in birds and constitute a vast reservoir of viruses that could potentially circulate in bird populations. All of the outbreaks of the highly pathogenic form to date have been caused by influenza A virus sub-types H5 and H7.
Migratory water birds - particularly wild ducks - are the natural reservoir of the avian influenza virus. These birds are also most resistant to infection. Domestic poultry, especially chickens and turkeys, are particular sensitive to epidemics of rapidly fatal influenza.
Direct or indirect contact between domestic birds and migratory water birds has often been responsible for epidemics. Live bird markets also play an important role in spreading it.
Recent research has shown that low pathogenic viruses can occasionally mutate and become highly pathogenic after being in circulation for a short time in a poultry population. During the 1983-1984 epidemic in the United States of America, the H5N2 virus which caused few fatalities initially, became highly pathogenic over six months with a mortality rate approaching 90%. In order to put an end to this epidemic more than 17 million birds had to be destroyed at a cost of almost $65 million US dollars. During the 1999 to 2001 epidemic in Italy, the original low pathogenicity H7N1 virus mutated in 9 months. More than 13 million birds either died or were slaughtered.
The conventional measures to combat spread to other farms and the virus becoming established in bird populations in the country are to quarantine infected farms and destroy birds which have been infected or potentially exposed. Apart from their highly contagious nature, the avian influenza viruses spread easily between farms by mechanical methods: contaminated materials, vehicles, food, cages, and clothing. These highly pathogenic viruses survived for long periods of time in the environment, particularly at low temperatures. Nevertheless, the strict health measures applied to farms can offer a degree of protection.
If measures to combat the infection are not taken promptly with high quality surveillance, the epidemics can last for several years. For example, an epidemic of the H5N2 virus began in Mexico in 1992. It was initially of low pathogenicity and progressed to a form of the disease causing high mortality rates and the epidemic was not ended until 1995.
A constantly mutating virus with two consequences.
All of the type A influenza viruses including those found regularly to be responsible for seasonal epidemics in human beings are genetically unstable and well suited to escaping the host's immune defence mechanisms. They do not have "identification" and repair mechanisms for errors that occurred during replication. As a result their genetic composition changes provided that they replicate in human beings or animals and a new antigenic variant soon replaces the original strain. The term antigenic "drift" is used for these constant and generally minor changes in influenza A virus.
This tendency for influenza viruses to permanently and frequently change their antigens means that they need to constantly monitor changes in the situation throughout the world and adjust the content of the influenza vaccinations annually. These have been two fundamental activities of the WHO worldwide influenza programme since it started in 1947.
The influenza virus had a second characteristic of considerable concern to public health. A viruses, including the sub-types of the different species are able to exchange, i.e. "reorganise" their genetic material and fuse. This process causes major antigenic "shift" which leads to the creation of a new sub-type that is different from the two viruses from which it was derived. As populations have no immunity against this new sub-type and with no vaccine to provide protection from it, in the past these major antigenic shifts have led to the emergence of pandemics with high mortality rates. In order for this event to occur, the new subtype must have genes from the human influenza virus that makes it possible for it to be transmitted easily and sustainably between people.
It has long been thought that conditions predisposing to the emergence of major antigenic shift are provided when human beings live in the immediate proximity of birds and pigs. As pigs are susceptible to infection from both the influenza virus and from mammal viruses, particularly human strains, they can act as the melting pot for the mixture of genetic material from human and avian viruses and the emergence of a new subtype. However, recent events have established a second possible mechanism. There are increasing findings that show that at least for some of the 15 subtypes of avian virus circulating in bird populations, it is human beings themselves who can act as the "melting point".
History of human infections by avian influenza viruses
Avian viruses do not normally infect species other than birds and pigs. The first documented case of human infection was in Hong Kong in 1997, when an H5N1 strain caused severe respiratory disease in 18 people, 6 of whom died. The infection coincided with an epidemic of highly pathogenic avian influenza caused by the same strain affecting poultry in Hong Kong.
Detailed investigations into this outbreak showed that most contact with infected living birds was responsible for the infection in human beings. Genetic studies subsequently found that the virus passed directly from birds to human beings. Transmission was limited to health workers and did not produce a serious form of the disease.
A rapid cull of all of the poultry in Hong Kong, approximately a million and a half birds according to estimate over three days, reduced the possibility of new direct transmission to human beings and appeared to have avoided a pandemic.
This event alarmed the health authorities. It was the first time that an Avian influenza virus had been transmitted directly to human beings and caused a serious disease with a high mortality rate. These concerns were brought to life again in February 2003, when an outbreak of H5N1 avian virus in Hong Kong caused two deaths and one death in a family that had recently returned to Southern China. Another child in the family died during this visit although the cause of death was unknown.
Two other avian viruses have also caused diseases in human beings. An outbreak of highly pathogenic H7N7 avian influenza started in the Netherlands in February 2003. Two months later this led to the death of a veterinary practitioner and produced mild disease in 83 people. Cases of mild avian H9N2 influenza occurred in Hong Kong children in 1999 (two cases) and mid-December 2003 (one case). H9N2 is not highly pathogenic to birds.
The most recent alert was in January 2004 when laboratory tests confirmed an avian H5N1 virus in people suffering from severe respiratory disease in North Vietnam.
Why is H5N1 of such concern?
Of the 15 subtypes of avian influenza virus, H5N1 is the most worrying for several reasons. It mutates rapidly and has a clear propensity to acquire genes from viruses that infect other species. Its ability to cause serious infection has been established on two occasions. Laboratory studies have also shown that isolates of the virus are highly pathogenic and may cause serious diseases in human beings. Birds that survive the infection excrete the virus for at least 10 years, both orally and in faeces, facilitating its spread through live poultry markets and by migrating birds.
The highly pathogenic avian influenza epidemic due to the H5N1 virus which began in mid-December 2003 in the Republic of Korea which is now seen in other Asian countries, therefore raises particular public health concerns. H5N1 varieties were also shown to be able to directly infect human beings in 1997, with a recurrence in Vietnam in January 2004. The spread of infection in birds has increased the possibility of direct infection of human beings. If the number of cases of human infection increases over time, the likelihood increases that people who are infected simultaneously by human and Avian strains will act as the "melting pot" for the emergence of a new sub-type with sufficient genes from the human virus so it can be transmitted between people easily. This would then mark the beginning of a new pandemic.
Can we avoid pandemics?
Based on historical trends, with the emergence of new sub-types of virus which transmit easily between people we can expect an average of three to four pandemics per century. However, it is impossible to predict the exact time when these will develop. In the twentieth century the major pandemic of 1918 - 1919, which caused 40 to 50 million deaths throughout the world according to estimates, was followed by two other pandemics in 1957-1958 and 1968-1969.
Experts agree that another influenza pandemic is inevitable and may be imminent.
Most influenza experts also recognise that the rapid slaughter of all of the poultry in Hong Kong in 1997 probably avoided a pandemic.
Several measures can be taken to minimise the public health risks of large outbreaks of highly pathogenic H5N1 avian influenza in birds. The immediate priority is to stop all spread in the poultry populations. This strategy helps to limit the possible exposure of human beings to the virus. Administration of effective vaccines against human strains circulating at the time to people who are highly exposed to a risk of coming into contact with infected poultry reduces the likelihood of concomitant infection of human beings with avian and human strains and therefore the risk of gene exchange. People who work in chicken abattoirs also need to be protected by equipping them with appropriate clothing and materials. They also need to be given prophylactic antiviral agents.
When cases of avian influenza develop in human beings, urgent information is needed about the extent of the infection in animals and in human beings and about human beings and about the circulating viruses in order for the public health risks to be assessed to decide on the best measures to take. A detailed enquiry into each case is also essential. Although the WHO, members of the worldwide influenza monitoring network, and other international bodies can help many of these activities, success in reducing these risks depends on epidemiological measures in the countries concerned together with their laboratories and the monitoring systems already in place.
Whist all these activities can reduce the likelihood of a strain responsible for a pandemic emerging, it is not possible to be sure that this can be avoided.
Clinical course of avian influenza H5N1 in human beings and treatment
Information published on this subject is limited to a study of cases occurring during the Hong Kong outbreak in 1997. Patients developed symptoms of fever, irritated throat, cough, and in the fatal cases, severe respiratory infection due to pulmonary viral infection. Adults and children who were previously in good health were affected as well as chronically ill people.
The tests to diagnose all influenza strains in human beings and animals are reliable and rapid. Many laboratories in the worldwide WHO network have sufficient biosafety installations and reagents to perform these and are very experienced in carrying them out. There are also rapid tests that can be performed at the patient's bedside to diagnose human influenza although these are not as precise as laboratory tests which are currently needed to fully understand the most recent cases and determine whether human infection is occurring either directly from birds or between people.
Anti-viral medicines, some of which can be used both for prevention and treatment are effective against influenza A strains in adults and children who are normally in good health, but these medicines do have limitations. Some of these are expensive and supply is limited.
There is also great experience in producing anti-influenza vaccines particularly because their composition changes every year, in order to adapt to antigenic drift of circulating viruses. However, at least four months are needed to produce large amounts of vaccine effective against a new viral sub-type.
Latest
Fill out my online form.



